Coarctation of the aorta
Download this information sheet as a PDF
The aim of this information sheet is to explain what coarctation of the aorta is, how it can be treated and what effect it may have on my child.
What is Coarctation of the Aorta?
Coarctation means a narrowing in the blood vessel wall. The aorta is the main artery carrying red (oxygenated) blood from the heart to the body. Coarctation of the aorta therefore describes the narrowing of the aorta. This means that the left ventricle has to work much harder than normal to push the blood through the narrowed blood vessel.
There is also a more severe condition called interrupted aortic arch (IAA) which always requires surgery. Interrupted means stopped. The aortic arch is the first part of the aorta, as it bends around the top of the heart. Interrupted aortic arch means that the aorta cannot carry red (oxygenated) blood to all parts of the body.
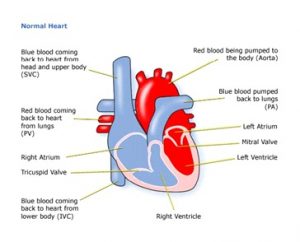
SVC: Superior vena cava
PV: Pulmonary valve
IVC: Inferior vena cava
PA: Pulmonary artery
Fig 2. Coarctation of the aorta
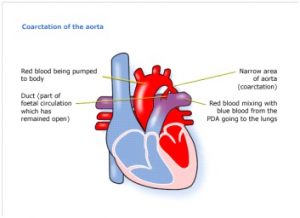
Figure 2 shows a heart affected by coarctation of the aorta. You can see where the aorta narrows before splitting in two. This narrowing affects blood flow where the arteries branch out to carry blood along separate vessels to the upper and lower parts of the body.
The duct is a connection between two main arteries (pulmonary artery and the aorta) and is present in all babies before birth and forms part of the foetal circulation. In healthy babies this closes off soon after birth, but in some patients with coarctation of the aorta it will remain open. Babies with an interrupted aortic arch rely on this duct for their blood to circulate, so if it starts to shut down they will become ill very quickly.
Figure 1 shows a healthy heart. The aorta is much wider than in the previous picture and the heart muscle around the left ventricle is thinner, as it does not have to work so hard.
How is coarctation of the aorta diagnosed?
Coarctation of the aorta or interrupted aortic arch can sometimes be seen on a scan during pregnancy.
If a baby has an interrupted aortic arch and has not been diagnosed before birth, they will be diagnosed during their first few days of life because they will become very ill and need urgent surgery.
If the aorta is very narrow, then children born with coarctation of the aorta will also become very ill and will usually be quickly diagnosed. If the aorta is not very narrow, then the child may not start to show symptoms for some years.
Older children may be diagnosed after they start to show symptoms such as pains in their legs, tiredness, headaches and dizzy spells. Sometimes there are no symptoms, but a heart murmur may be heard during a routine examination.
Some children with coarctation of the aorta also have other heart disorders, such as a ventricular septal defect (VSD), or an aortic stenosis, which is a narrowing around the entrance to the aorta.
The following tests and examinations may be used to confirm diagnosis:
- pulse, blood pressure, temperature, and number of breaths a baby takes a minute
- listening with a stethoscope for changes in the heart sounds
- an oxygen saturation monitor to see how much oxygen is getting into the blood
- a chest x-ray to see the size and position of the heart
- an ECG (electrocardiogram) to check the electrical activity
- an ultrasound scan (echocardiogram) to see how the blood moves through the heart
- checks for chemical balance in blood and urine
- a cardiac catheterisation or MRI (Magnetic Resonance Imaging) scan may be needed
Treatment
If a baby needs treatment for coarctation of the aorta or an interrupted aortic arch, then they will need to have surgery. The surgery will widen the artery or fill in the missing section. Stents and catheters may also be used in this situation. Today, more and more babies are being diagnosed with coarctation of the aorta antenatally (before birth). Once the baby is born they are given prostaglandin, a medicine which allows the duct to remain open until surgery is performed.
Coarctation of the aorta in older children can be treated either with or without surgery. The non-surgical method uses a balloon catheter (tube) or stent (metal cage).
A catheter can then be threaded into the heart via a vein and into the aorta past the narrowed area. A balloon on the end of the catheter is then inflated and pulled back to stretch the narrow part of the aorta. In older children a stent can be inserted over the balloon and left at the place where the artery was too narrow to keep the aorta wide open.
The other option is to have surgery which will widen the aorta at the point where it is too narrow.
Surgery on the aorta is done through the left side of the chest, and the heart continues beating throughout the operation.
If your child has other heart defects, the surgery needed will depend on how the heart can best be modified to cope with the problems they have.
This kind of surgery has the risk of a blood clot after angioplasty. Also, surgery takes place close to the spine so there is a slight risk of damage to the nerves. The cardiologist or surgeon should discuss the risks with parents or carers before asking them to consent to the operation.
The length of time in hospital will usually be only a week or so, of which one or two days will be spent in the intensive care and high dependency units. Of course, this depends on how well your child is before and after the surgery, and whether there are any complications.
Some children with the condition may be able to be treated with the control of high blood pressure through a combination of diet, exercise and medication.
How will the child be affected?
Most children are completely well, active, and gaining weight a few days after surgery. They will have a scar on the left side of the chest and there may be smaller scars on the hands and neck, which will usually fade away.
Sometimes the coarctation reoccurs – this is more common after a balloon catheter than after surgery. Children therefore need regular follow-ups to make sure their condition is monitored closely.
Evidence and sources of information for this CHF information sheet can be obtained at:
(1) NHS Choices. Congenital heart disease. London: NHS; 2017. Available at:
https://www.nhs.uk/conditions/congenital-heart-disease/treatment/#COA
(2) National Institute for Health & Care Excellence. NICE interventional procedure guidance IPG74. Balloon angioplasty with or without stenting for coarctation or recoarctation of the aorta in adults and children. London: NICE; 2017. Available at:
https://www.nice.org.uk/guidance/IPG74/chapter/2-The-procedure#safety
(3) American Heart Association. Coarctation of the aorta. Available at:
(4) Hu ZP, et al. Ann Vasc Surg. 2014;(28):394-403
(5) Turkay S, et al. J Cardiovasc Dis Res. 2010; (1):181-90
(6) Matsui H, et al. Circulation. 2008; (118):1793-801.
(7) Fiore AC, et al. Ann Thorac Surg. 2005;(80):1659-1664
About this document:
Published: June 2015
Reviewed: May 2022
To inform CHF of a comment or suggestion, please contact us via info@chfed.org.uk or Tel: 0300 561 0065.









