Pulmonary Stenosis
Download this information sheet as a PDF
The aim of this information sheet is to explain what pulmonary stenosis is, what effect it will have on a child and how it can be treated.
What is pulmonary stenosis?
Pulmonary means ‘lungs’ and stenosis means ‘narrowing’, therefore pulmonary stenosis describes a condition where the pulmonary valve is very narrow. When this condition is present the muscle of the right ventricle must work harder to pump the blood through the narrow valve. Depending on how narrow the valve is, a child may have no symptoms, may tire quickly, or even faint.
Animation of normal heart

Animation of pulmonary stenosis
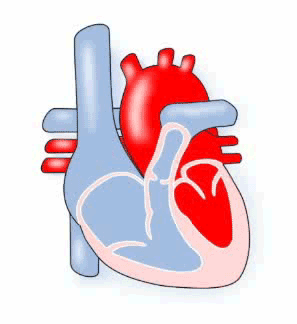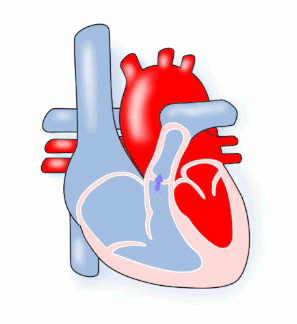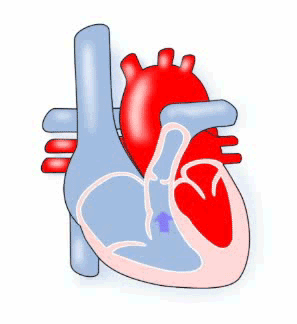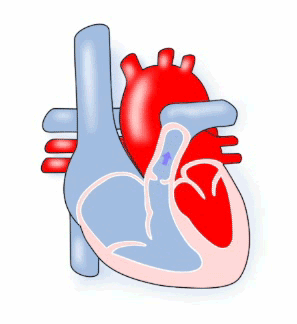
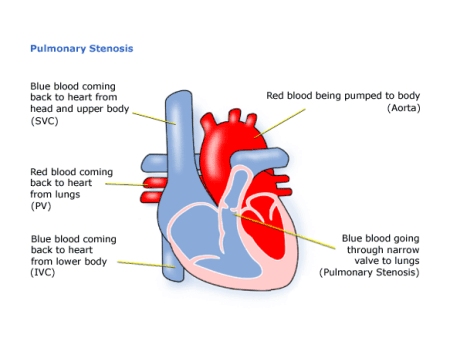
Diagram of Pulmonary Stenosis
How is pulmonary stenosis diagnosed?
Your child’s pulmonary stenosis may have been diagnosed during a scan in pregnancy. In most cases pulmonary stenosis is only diagnosed after birth. After birth the sound of blood moving through the narrow valve can often be heard as a heart murmur (a heart murmur is an extra or unusual sound heard during a heartbeat). Sometimes pulmonary stenosis can occur with other heart abnormalities.
When a heart problem is suspected the following tests may be done to identify the problem:
- pulse, blood pressure, temperature, and number of breaths a baby/child takes a minute
- listening with a stethoscope for changes in the heart sounds
- an oxygen saturation monitor to see how much oxygen is getting into the blood
- a chest x-ray to see the size and position of the heart
- an ECG (electrocardiogram) to check the electrical activity
- an ultrasound scan (echocardiogram or ‘echo’) to see how the blood moves through the heart
- blood and urine tests
- a cardiac catheterisation or MRI (Magnetic Resonance Imaging) test may be needed.
What happens after diagnosis?
You, your GP and health visitor should have details of your baby’s or child’s condition from the heart doctor (paediatric cardiologist). If not, call the hospital at which your child was seen, ask for the name of the paediatric cardiologist and their telephone number. Call and explain that you need the information to pass on to, for example, your local accident and emergency department should he or she have a sudden illness.
You should have the number of a cardiac liaison nurse or outreach nurse to hand should you have questions or any fears about your child’s heart problem
You should have the number of a parent support group.
How is pulmonary stenosis treated?
The treatment depends on how narrow the pulmonary valve is; most children do not require any surgery. In many cases pulmonary stenosis does not cause any symptoms, but a cardiologist will need to keep an eye on the condition to ensure that it does not get worse. Changes can occur slowly and appointments can be infrequent depending on the condition.
Severe narrowing of the pulmonary valve will cause the right ventricle to work harder to pump blood through the pulmonary valve. If your child has a severe narrowing of the pulmonary valve, they may tire more quickly or even faint and require treatment.
If your child has other heart defects, the kind of surgery needed will depend on how the heart can best be modified to cope with all the problems he or she has. For most children the procedures are low risk but this can depend on your child’s general health. The doctors will discuss risks with you in detail before asking you to consent to the operation.
There are two common procedures used to treat severe pulmonary stenosis:
Balloon dilation or balloon valvoplasty:
The aim of the procedures is to make the entrance to the pulmonary artery bigger, allowing the blood to be pumped to the lungs at lower pressure. A tube is inserted through a vein in the groin leading into the heart. The tube is then passed through the narrow valve into the pulmonary artery. A balloon on the end of the tube is inflated, thereby stretching the pulmonary valve. This does not leave any scarring and recovery time is usually overnight, so your child only spends one or two days in hospital.
Corrective surgery:
In very severe cases open heart surgery may be needed – the heart will need to be stopped and opened to be repaired. This means that a machine will have to take over the job that the heart normally does – the heart bypass machine.
The aim of the operation is to enlarge the area around the pulmonary valve, sometimes needing a valve replacement. The valve used to replace the child’s narrow valve is usually a homograft (a valve donated from another person). These valves commonly need to be replaced after several years. The length of time in hospital after surgery will usually be only 5 to 7 days, of which one or two will be spent in the intensive care and high dependency unit. Of course this depends on how well your child is before and after the surgery, and whether any complications arise.
How will the treatment affect my child?
Most children are completely well, active, and gaining weight a few days after a balloon catheter or surgery. After surgery he or she will have a scar down the middle of the chest, and there may be small scars where drain tubes were used. These fade very rapidly in most children but they will not go altogether.
Smaller scars on the hands and neck usually fade away completely.
It is common for the pulmonary valve to leak and it may need further repair or replacement.
Evidence and sources of information for this CHF information sheet can be obtained at:
(1) National Institute for Health & Care Excellence. Pulmonary Valve Stenosis.
Balloon dilation of pulmonary valve stenosis. Guidance IPG67. London: NICE; 2017. Available at:
https://www.nice.org.uk/Guidance/ipg67
(2) Great Ormond Street Hospital. Pulmonary Stenosis Information. London: GOSH; 2017. Available at:
www.gosh.nhs.uk/medical-information-0/search-medical-conditions/pulmonary-stenosis
About this document
Published: December 2014
Reviewed: May 2022
To inform CHF of a comment or suggestion, please contact us via info@chfed.org.uk or Tel: 0300 561 0065.









